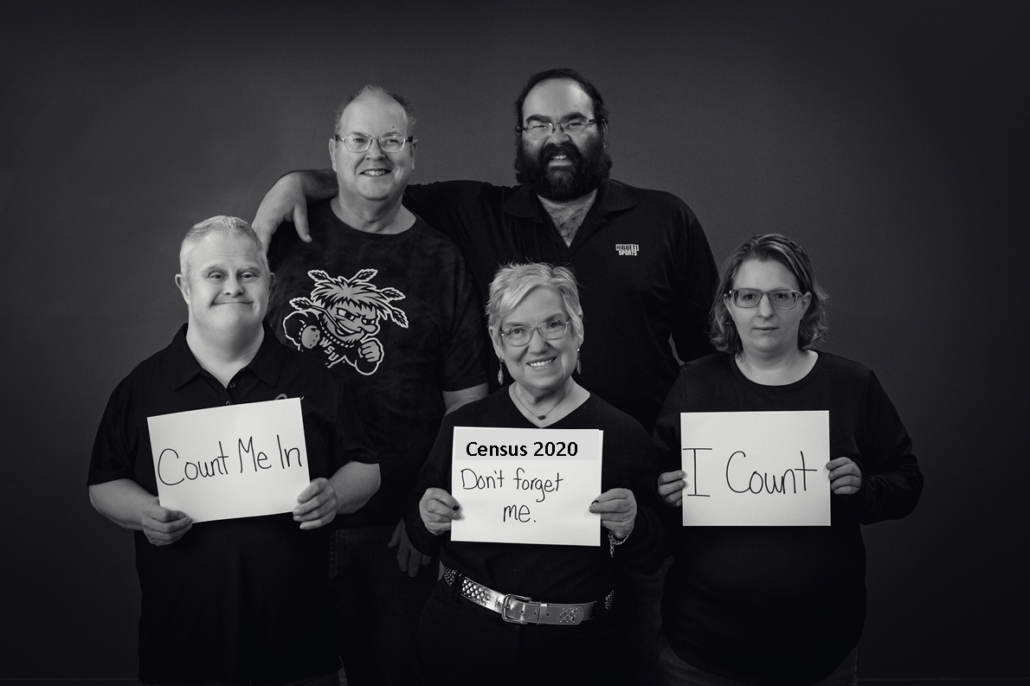High Risk, Infected, and Dying of COVID-19, but Who Is Counting?
By Nicole Jorwic, Senior Director of Public Policy
At an institution in Denton, Texas, where 400 people with disabilities live, 54 have COVID-19, and 50 employees are infected.
At a state run facility in Danvers, Massachusetts, 40% of residents are infected, plus 55 nurses who work at the facility.
In Illinois, two institutions are experiencing such extreme outbreaks that the National Guard is being called in to help with temperature checks.
And in New York, Maryland, Washington State, Georgia, and most likely in every state – people with intellectual and developmental disabilities, or I/DD, have lost their lives to this vicious virus.
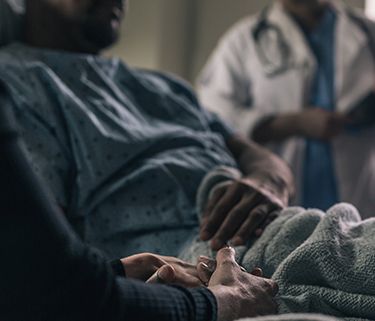
People with I/DD face grave danger in the face of the COVID-19 pandemic – with underlying health conditions, many are at a higher risk. Then why aren’t you hearing about it? Nursing homes and cruise ships, overflowing emergency rooms and makeshift hospitals set up in Central Park fill our television screens and headlines. Why are people with disabilities far too often ignored when we are focusing on who is impacted by this crisis? Who is counting – and revealing – the dangers facing people with intellectual and developmental disabilities, particularly those living in large, congregate settings?
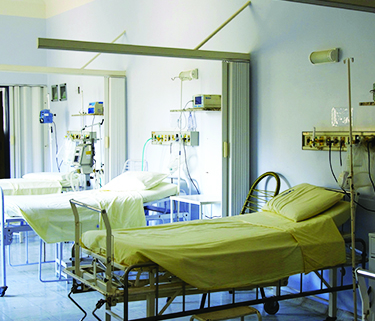
You see, in 2020, in 36 states, tens of thousands of people with I/DD live in institutions. These settings are called many things, like Intermediate Care Facilities for People with Intellectual and Developmental Disabilities (ICFs), “state schools,” “state operated developmental centers” or “state hospitals.” And, thousands of people with I/DD live in nursing homes too.
COVID-19 is running through these large facilities in every state like a wildfire, but where is the outrage? Does the general public believe that these places shut down decades ago? Or is it because these institutions are not publicly reporting what is happening to the residents and staff?
Information about the tremendous risks posed by this pandemic to people with disabilities, whether they live in an institution or nursing homes, must be captured. The Centers for Medicare and Medicaid Services just announced that they are requiring nursing homes to report cases and deaths from COVID-19 to the Federal government. But that requirement was not extended to ICFs or institutions for people with disabilities, nor does it require data from nursing homes that tracks whether or not a sick or deceased individual had a disability. CMS must extend these same requirements to all institutional settings, including ICFs, institutions, and nursing homes, and require that people with disabilities are specifically tracked in this data collection.
For my entire life, the disability community has been fighting to complete what began decades ago with the families and individuals with disabilities fighting to get people out of institutions. We must create the capacity for a home and community-based service (HCBS) delivery system to serve all who need supports. We must build up the workforce needed to provide those services and create the flexible supports that people need so that people with disabilities can be safe in their homes and communities.
We will get there by investing in HCBS. Representative Debbie Dingell and Senator Bob Casey have introduced bills to create grants for states to expand these services during the pandemic, and pay the workforce that provides those services what they should be paid to do the important work they do, providing support for as much independence as possible in the community.
Congress must include those HCBS grants to states in the next COVID-19 response legislation to keep people with disabilities out of dangerous congregate settings and in their homes and communities. And when this is over, I won’t rest until we have the reckoning that this country needs to fully understand where people with disabilities belong: safely integrated in their homes and communities.
If we are all in this together, then we all count.